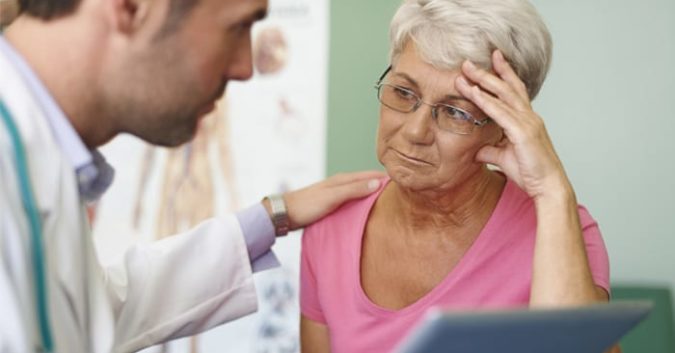
A long time ago, before the great discoveries of modern medicine, the most physicians could offer a suffering patient were a pair of ears and empathy. Now, we have the immense knowledge and impressive technology needed to make amazing things happen in healthcare.
But some technological advancement might be more of a hindrance than a help. In fact, it may be one of many underlying causes of medical errors.
Today’s explosion of medical advances has created a “separation between the science of medicine and the humanism and compassion of medicine,” said Lloyd Minor, M.D., dean of the Stanford School of Medicine, who believes doctor-patient relationships are integral to the wellbeing and treatment of patients.
In a recent article, Minor and other Stanford doctors explored how the doctor-patient relationship has changed over the past decades, and why we’re better off taking lessons from the grandfathers of medicine.
‘Listening Is Crucial to Good Healthcare’
Most clinicians agree that the fast-paced, innovation-driven demands of healthcare cut into time they could be spending with patients, said Donna Zulman, M.D., Stanford’s assistant director of medicine. It’s difficult enough just to keep up with the latest medical research, technology, and treatment options.
Zulman points to 2 main barriers to meaningful connections: short appointments and electronic health records (EHRs). Fifteen-minute appointment limits, added to time-consuming, highly regulated EHR upkeep, means clinicians spend more time managing patient information than actually talking to patients themselves.
Doctors got into medicine “to learn and apply science for the benefit of patients,” said Kelley Skeff, M.D., Ph.D., professor of medicine at Stanford. “But their connections to science and to the patient are commonly impeded by the requirements of the system. And those who are the most empathetic may, in fact, burn out faster as their self-care is neglected.”
And when doctors burn out, all manner of things can go wrong.
Why Is the Doctor-Patient Relationship So Important?
The reason for forming more meaningful relationships is clear, said Zulman: Good communication results in fewer medical errors.
The consequences are clear, too. Without a bond with their patients, doctors risk misdiagnosing conditions, providing unnecessary or unwanted treatment, fragmented patient care, and ultimately, burning out.
Physician burnout, another key cause of medical mistakes, is at an all-time high. A recent Medscape survey found 42 percent of doctors experience burnout in the form of emotional exhaustion, cynicism, and ineffectiveness – a cocktail for serious medical disaster. A Stanford study reported a burnout rate as high as 54 percent, up from 46 percent in 2011.
This increase in burnout rates may explain the exponential rise in rates of medical error. Estimated to kill a quarter of a million American patients in 2016, medical errors now lead to as many as 440,000 deaths per year. That makes medical malpractice the third-leading cause of death in the United States. And thanks to gaps in reporting, even that might be an underestimation.
How to Start a Life-Saving Conversation
It’s hard to believe that the people responsible for saving our lives could claim them, but medical malpractice has disastrous effects on patient care. If the answer to reducing errors is as simple as lending an ear to patients’ concerns, then what is the healthcare industry waiting for?
Stanford has come up with a few solutions to help doctors practice good communication: a workshop for role-playing patient interactions; Stanford Presence 5 research, based on observations of real-life interactions; and the Coordinated Care program, focused on reducing hospitalizations among chronically ill patients by making them “partners in their own wellness.”
However, said Zulman, “It’s actually a really challenging problem.”
Improving communication will mean better integrating technology with medicine so that health professionals take less time to access and share patient data. It will mean encouraging doctors to look for subtle clues to patients’ values and cultures, like how they decorate their hospital rooms. It will mean ensuring all doctors, no matter how pressed for time or disinclined to socialize, sit down and really listen to what their patients care about.
Only through the information patients reveal about themselves can doctors answer the most important question in medicine: What does the patient need most? Empathy never gets old, especially when patients’ lives are on the line.